Corticosteroids: Uses, Benefits, and Risks
March 7th, 2017 | 4 min. read


Corticosteroids refers to a class of hormones that occur naturally in the body’s adrenal glands; however, these hormones can also be synthetic — manufactured in a lab. Both can be used medicinally to treat a variety of health conditions, including orthopedic conditions like arthritis and inflammation from soft tissue injuries.
Two chemical classes of corticosteroids exist:
Glucocorticoids have effects on metabolism, immune response, cell creation and turnover, and the constriction of blood vessels. Glucocorticoids can help to fight inflammation and suppress hypersensitive white blood cell responses to infection and other threats. These corticosteroids also affect blood pressure and skin cell production.
Cortisol (hydrocortisone) is a naturally-occurring glucocorticoid. Prednisone, commonly prescribed for a variety of health issues including asthma and allergies, is an example of a synthetic or human-made glucocorticoid.
Mineralocorticoids regulate the balance of water and electrolytes in the kidneys. Aldosterone is a naturally-occurring mineralocorticoid. Fludrocortisone (Florinef) is an example of a synthetic version of the same.
Collectively, these two classes of corticosteroids are used to treat many different health conditions, including allergies (skin responses, respiratory reactions, anaphylaxis), endocrine issues, gastrointestinal problems, rheumatological diseases, certain autoimmune diseases like lupus, eye problems, inflammation from injury, and more.
Pharmaceutical corticosteroids can come in a few different forms:
- Inhalers and sprays
- Injectables or IV
- Oral (pills)
- Topicals (creams and ointments)
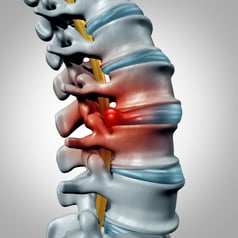
Orthopedic Uses of Corticosteroids
In orthopedics, injectable corticosteroids are often used for their anti-inflammatory properties. For some painful conditions, for example arthritis or a bulging disc, an orthopedist may suggest one or more injections to the joint or the site of injury in order to bring down swelling, inflammation, or pain.
Generally, this course of treatment is used conservatively; too much or too frequent use of injectable corticosteroids can lead to side effects (see below, “Risks”).
Conditions that may benefit from cortisol or hydrocortisone injections include:
Bursitis. The fluid-filled bursa, or sac, that acts as a cushion between bones and soft tissue can sometimes become irritated, inflamed, or swollen. Pain and limited motion can result. Bringing down the swelling and irritation can reduce pain and restore mobility. Aspiration of collected fluid, followed by corticosteroid injection is an option for treatment.
Osteoarthritis (OA). Treatment of OA is probably one of the most common uses of corticosteroids in orthopedics. When cartilage wears away, pain and inflammation in the joints is common. A corticosteroid injected into the affected area may provide temporary relief from these symptoms. The goal of treatment is pain control and restored function. Pain relief may last several weeks, or several months, depending on the severity of the disease. Because overuse of corticosteroids carries a number of risks, people with OA should talk to their doctors about other, ongoing forms of symptom management
Lower back pain. Injectable corticosteroids can help with pain relief in the case of conditions like spinal stenosis (a compression of the spaces in the spine), pinched nerves, and ruptured discs. Sometimes pain relief is lasting, but other forms of therapy or surgery may be advised for long-term pain and symptom management — especially if the symptoms are caused by disc degeneration from osteoporosis or OA. (In some cases, spinal fusion surgery may be recommended.)
Neck pain (cervical radiculopathy). A pinched nerve in the neck vertebrae can lead to a radiating pain felt in the neck, shoulder, arm, or even the hands. This pinching can be caused by a compression of the vertebrae, a bulging disc, or a ruptured disc. A corticosteroid injection can bring down the swelling while the injury heals. However, in the case of disc degeneration due to osteoporosis or OA, other forms of therapy or surgery may be worth talking about with a doctor.
Tendonitis. This inflammatory condition — often the result of overuse or repetitive strain — can lead to pain and swelling in the tendons and soft tissues. Tendonitis is especially common in the elbow (tennis elbow), the shoulders, the knees, and the wrists. Injections may bring some relief from severe or disabling pain.
Benefits of Corticosteroids
There are some definite advantages to using corticosteroid treatment for inflammatory musculoskeletal conditions. These include:
- Near-instant pain relief
- Rapid reduction in inflammation
- Permanent cure, sometimes, in the case of a localized injury
- A high success rate
When symptoms are disabling — for example, if your Achilles tendonitis hurts too badly to walk, or your tennis elbow is so severe you can’t write, type, use the phone, or hold a fork — a cortisone injection may bring relief from an intolerable level of pain and swelling, long enough to make you comfortable while your body heals.
However, there is a downside. This form of medication can’t be used indefinitely to manage pain and swelling in chronic or recurring conditions. If symptoms return after a few weeks, a second shot may not be safe. To avoid damaging side effects, orthopedists usually limit the administration of these injectables to 3 to 4 shots per year.
Corticosteroid Risks
 Though a limited dose of corticosteroids can help reduce pain and inflammation, taking them does present risks.
Though a limited dose of corticosteroids can help reduce pain and inflammation, taking them does present risks.
The very reasons they work so well at reducing pain and inflammation are the same reasons they’re dangerous if taken too frequently or in large quantities.
Corticosteroids suppress the immune system and the creation of white blood cells, halting immune system “overreactions” that create pain and swelling. But remember, inflammation and histamine responses to allergens are all natural processes for fighting off infections and other immune system attacks. Even pain serves a purpose; it tells you to slow down and rest.
Suppressing the body’s ability to do what it’s meant to do can lead to further harm. Remember, corticosteroids are not meant to be a long-term solution to a tissue injury.
The risks of treatment can include:
- Temporarily elevated blood sugar levels, particularly for diabetic patients
- Infection or bleeding at the injection site
- Insomnia/ agitation
- Palpitations, hot flashes, flushing, mild mood disturbance
- Post-injection flare: a temporary increase in pain at the injection site
- Thinning or discoloration of the skin at the site of injection
- Localized subcutaneous fat atrophy
- Weakening of tendons
- Avascular necrosis (bone death), extremely rare
Long-term use of steroids can lead to cataracts, high blood pressure, stomach ulcers, and osteoporosis, among other issues. Some side effects that you may have heard of, including weight gain, acne, and diabetes, occur with long term oral use of steroid medication, but generally do not occur with periodic injection treatments.
The good news is, very infrequent use of injected steroids is unlikely to cause serious side effects. Even so, before getting a shot it’s wise to talk to your doctor about any pre-existing conditions you may have and how the injection may affect them.
Summary: Pros and Cons of Corticosteroids
For inflammatory conditions like arthritis, muscle strains, tendonitis, bursitis, or pinched nerves, injectable corticosteroids can help to rapidly reduce inflammation and pain. They have a high success rate and can bring relief more quickly than oral anti-inflammatory drugs like NSAIDs.
However, this form of therapy is not without risks. Though sometimes pain relief is permanent, in some cases the symptoms will return after a few weeks or months. Due to the risks of prolonged steroid use, it’s generally unwise to receive more than 3 to 4 injections per year.
If you feel that you might need to see an orthopedic specialist about your chronic pain issues, feel free to reach out to Coastal Orthopedics in Corpus Christi, Texas at (361) 994-1166 or simply click the button below to request an appointment today!
Article written by: Rob Williams, MD
Dr. Williams has been practicing orthopedic surgery in Corpus Christi since 1998. After graduating from Texas Tech hereceived his medical degree from the University of Texas at San Antonio. At the prestigious Campbell Clinic located at the University of Tennessee, Dr. Williams completed not only an Orthopedic Surgery Residency, but an additional year of Fellowship Training in Spine Surgery. Dr. Williams is dedicated to creating an excellent patient experience in the office or in the surgery suite.
Topics:

