Topics:
Search for topics or resources
Enter your search below and hit enter or click the search icon.
April 26th, 2019 | 4 min. read
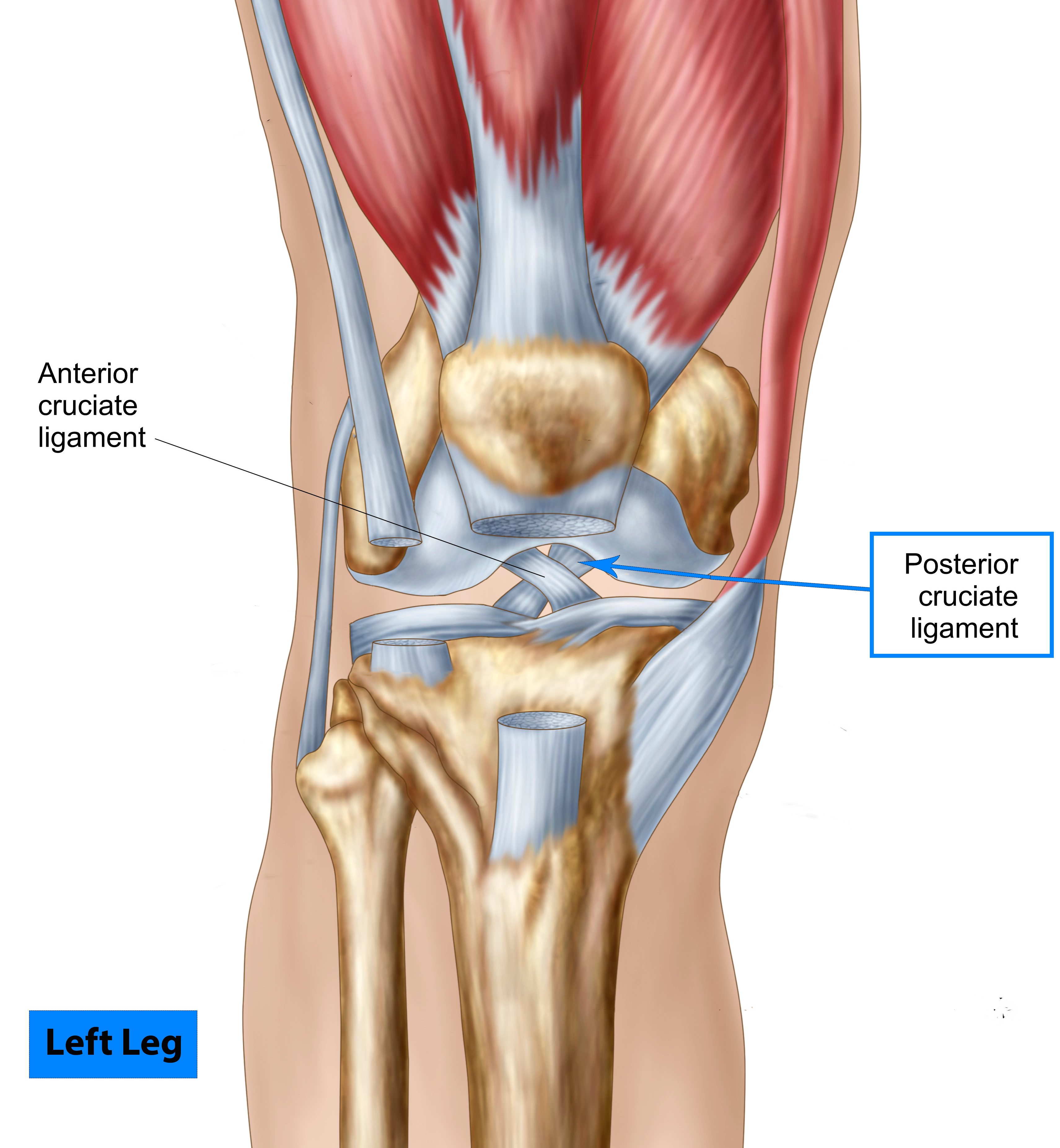
.jpg?width=231&name=storyblocks-anatomy-of-human-knee-joint_H60CxB5AZ%20(1).jpg) The posterior cruciate ligament (PCL) is a tough fibrous band of tissue that works within the knee. Together with the anterior cruciate ligament (ACL), the two bands criss-cross each other inside the knee in order to provide stability. There is also the medial collateral ligament and the lateral collateral ligament which sit on the middle side of the knee and the outer-side of the knee, respectively. Together, these ligaments connect the femur to the tibia, forming the knee joint. It is very important to be mindful of the health of these ligaments since damage to these tissues can cause severe pain and affect further usage of the knee. While each of these four ligaments is crucial to the function and stability of the knee, we will specifically be addressing issues of the PCL for this blog post. These issues include, risks present to the ligament, ways to prevent injuries, treatment for injuries, and of course the PCL injuries themselves.
The posterior cruciate ligament (PCL) is a tough fibrous band of tissue that works within the knee. Together with the anterior cruciate ligament (ACL), the two bands criss-cross each other inside the knee in order to provide stability. There is also the medial collateral ligament and the lateral collateral ligament which sit on the middle side of the knee and the outer-side of the knee, respectively. Together, these ligaments connect the femur to the tibia, forming the knee joint. It is very important to be mindful of the health of these ligaments since damage to these tissues can cause severe pain and affect further usage of the knee. While each of these four ligaments is crucial to the function and stability of the knee, we will specifically be addressing issues of the PCL for this blog post. These issues include, risks present to the ligament, ways to prevent injuries, treatment for injuries, and of course the PCL injuries themselves.
The PCL works essentially as an elastic anchor, keeping the tibia from moving too far back in relation to the femur. The properties of this ligament ensure this capability. The PCL is both strong and flexible. It is not without limitations however and when too much pressure is put on the PCL it can be stretched or torn. This type of injury to a ligament is known as a sprain. One of the most common causes of this sprain is a forceful impact to the front of the knee while it is flexed (bent). One main culprit of this is automobile accidents. It is highly likely if you are sitting in the passenger’s side of a vehicle when a collision occurs, that your knee or both will hit the dashboard causing a PCL injury. Sports also cause many PCL injuries. It is easy to sustain a PCL sprain for instance, if you are running down the football field and get “chop-blocked”. It happens very often at all levels of play. Non-contact sports such as basketball and soccer are also full of risks to the knees. Even the seemingly simple movement of a golf swing can cause a PCL injury through the twisting motion of the leg as the player follows through. While PCL injuries caused by twisting are more rare, it is important to be mindful of the risks present. And while the risks are plenty they can be mitigated by:

If you suspect that you have sustained a PCL sprain it is crucial to look for the symptoms:
It is possible to have a sprain and not realize it because the symptoms can be subtle for minor PCL injuries. It’s very hard to miss the symptoms of the more severe sprains however.
Like any other ligament of the body, PCL sprains are classified according to a traditional grading system:
In general, for all grades of PCL injuries, the initial treatment is to follow the RICE rule. That is:
The doctor may also recommend a non-steroidal anti-inflammatory drug (NSAID) to relieve minor pain and swelling. After initial treatment with the RICE method, further treatment of a PCL injury depends on the severity.
The duration for a PCL injury also depends on the severity of the sprain, but typically full recovery is achieved between 4 to 12 months.
If your knee exhibits signs of a knee sprain it should be a priority to consult with your doctor to figure out if you have a PCL injury. A diagnostic examination of the knee will begin with your doctor maneuvering your knee in ways to test the strength of the PCL and see if your tibia slides back when the knee is flexed. If the doctor suspects a PCL sprain an x-ray exam will be ordered. While soft tissues aren’t especially visible in an x-ray, it is possible that your PCL will pull a piece of bone off from the anchor point. This “floating” fragment of bone is visible with an x-ray and is a tell-tale sign of a Grade 3 sprain. Further imaging will likely be ordered in the form of an MRI exam. An MRI is especially helpful in visualizing soft tissue injures such as a PCL sprain. After this your doctor will discuss the best treatment options for your injury and come up with a plan best suited to get you back to your regular activities as quickly and safely as possible.
Coastal Orthopedics is an excellent choice for treatment of all types of bone and joint injuries, such as a pesky PCL sprain. Feel free to call and set up an appointment so our talented and knowledgeable staff can help get you back to a healthy and active lifestyle!
Dr. Williams has been practicing orthopedic surgery in Corpus Christi since 1998. After graduating from Texas Tech hereceived his medical degree from the University of Texas at San Antonio. At the prestigious Campbell Clinic located at the University of Tennessee, Dr. Williams completed not only an Orthopedic Surgery Residency, but an additional year of Fellowship Training in Spine Surgery. Dr. Williams is dedicated to creating an excellent patient experience in the office or in the surgery suite.
Topics: