Platelet Rich Plasma Therapy (PRP): Process and Procedures
March 28th, 2017 | 4 min. read


Platelet-Rich Plasma Therapy (PRP) is a process by which a patient's own blood is concentrated and then used to speed the healing of chronic tissue injuries, including tendinitis, sprains, and some milder forms of arthritis....so how does it work?
How Does PRP Therapy Work?
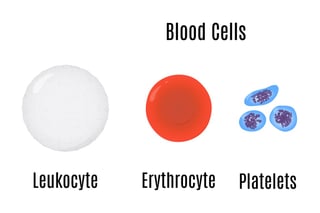 Platelets (also called thrombocytes) are one of three types of cells in our bloodstream, along with red blood corpuscles (erythrocytes) and white blood cells (leukocytes). Red cells carry oxygen and carbon dioxide; white cells combat infection; and platelets enable clotting and promote healing of injured body tissues. When you cut your finger, platelets are the cells that make it possible to stop the bleeding, block the cut, and allow your body the chance to close the cut.
Platelets (also called thrombocytes) are one of three types of cells in our bloodstream, along with red blood corpuscles (erythrocytes) and white blood cells (leukocytes). Red cells carry oxygen and carbon dioxide; white cells combat infection; and platelets enable clotting and promote healing of injured body tissues. When you cut your finger, platelets are the cells that make it possible to stop the bleeding, block the cut, and allow your body the chance to close the cut.
Platelets contain proteins, called growth factors, which allow them to perform these actions. Without them, the body cannot signal itself to run in “healing mode,” which means that without platelets, your body would be unable control inflammation, heal tissues, or build new skin. In addition, platelets increase the production of collagen and stimulate blood flow, essential components in the body’s healing process.
PRP therapy aims to magnify the power of the platelet. By collecting and concentrating platelets into a single injection, an injured body part may benefit from up to five times as many growth factors than is contained in normal whole blood. Best of all, the blood comes from your own supply—eliminating any risks or mismatch, infection, contamination, or other problems that might lead to rejection.
What Are the Most Common Injuries Treated by PRP Therapy?
Any injury involving a partial tear to a tendon (the tissue connecting bones to other bones) or ligament (the tissue connecting 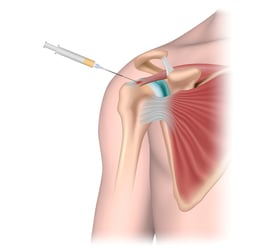 muscles to bones) may benefit from a platelet-rich infusion. Complete tears and ruptures must be treated with surgery, although PRP therapy could in theory help speed the healing process after a restorative surgical procedure.
muscles to bones) may benefit from a platelet-rich infusion. Complete tears and ruptures must be treated with surgery, although PRP therapy could in theory help speed the healing process after a restorative surgical procedure.
The most common usages of PRP therapy occur in injuries to the shoulder, knee, and elbow, including arthritic knee joints,
rotator cuff tears, severe hamstring pulls, quadriceps injuries, and damage to the Achilles tendon behind the ankle.
What Is the PRP Therapy Process?
PRP therapy is a relatively simple process that can be performed in under two hours. It does not require hospitalization, and may be done as an outpatient procedure.
Unlike blood tests, where the patient is generally instructed not to eat or drink for up to 12 hours before, no preparations are required for PRP therapy. The patient is only recommended to hydrate well in advance, as higher levels of water in the body will make drawing blood easier for the doctor.
If you use corticosteroids or NSAID anti-inflammatory medicines, such as ibuprofen (Motrin) or naproxen (Aleve), you will be required to have stopped taking them up to a week before PRP therapy, and not to resume use of these types of medications immediately afterwards. They will interfere with PRP therapy and possibly nullify any results.
The steps involved in PRP therapy are:
- Step 1: Collect the patient’s own blood.
Less than two ounces (between 15 to 50 milliliters) are required for the procedure. The collection is virtually identical to giving blood for a blood test, with a collection needle inserted into a vein in the arm and the blood captured in a small vial.
giving blood for a blood test, with a collection needle inserted into a vein in the arm and the blood captured in a small vial. - Step 2: Centrifuge the blood.
A centrifuge is a device that spins at high speeds. This action physically separates the solid and liquid parts of the blood: red blood cells (erythrocytes), white blood cells (leukocytes), platelets (thrombocytes), and plasma (liquid). - Step 3: Process and collect the platelets.
Regular blood contains about 200,000 platelets per milliliter, while platelet-rich plasma contains as much as five times that amount. The resulting three to seven milliliters of platelet-rich plasma will be collected in a syringe, to be administered immediately. - Step 4: Inject the PRP into the desired site.
The final syringe of platelet-rich plasma will contain approximately 1-2 teaspoons of fluid. With the guidance of an ultrasound probe, the PRP will be guided into the proper location, based on the nature of the injury being treated.
What Is the Procedure to Inject PRP?
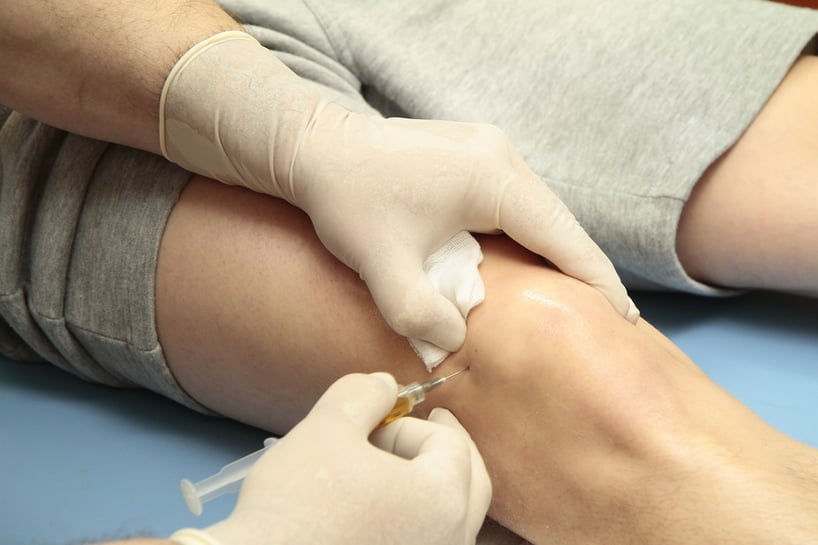
The actual procedure of injecting platelet-rich plasma into an injury site first requires basic cleansing with alcohol, iodine, or Betadyne to ensure the skin is free of potential infection-causing microorganisms.
As the procedure may take several minutes to complete, a local anesthetic will be used to ensure the patient is as comfortable as possible. Traditionally an anesthetic is injected into the affected location, and then given about fifteen minutes to take full effect.
Alternatively, ultrasound probes may be used to initiate what is called a “nerve block” for the same effect without an additional injection. The ultrasound nerve block may also be necessitated by the patient’s physical condition, the location and nature of the injury, or the patient’s personal preference.
To ensure the PRP is injected into the precise location required, ultrasound will be utilized to visualize the inside of the body, and to guide the doctor’s hand. A small amount of ultrasound gel will be applied to the skin over the affected site, and then a small ultrasound probe, or wand, will be pressed to the area. The resulting image will be transmitted directly to a screen.
If the injured body part contains scar tissue, that tissue will need to be punctured multiple times to create pathways for the PRP to permeate. This procedure is called PNT, or percutaneous tenotomy. In addition, this procedure can break up bone spurs and calcified pieces within a tendon, which despite being left inside the treatment site should not present any problems for the procedure or the healing process.
The plasma-rich platelets will now be injected into the joint capsule or other location. Once complete, the needle puncture will only require simple blotting and bandaging.
What Post-operative Care Is Required for Platelet Rich Plasma Therapy?
Patients who undergo PRP therapy should be able to return to normal everyday activities almost immediately. As the injection of PRP fills the injury site with fluid, it is normal to perceive the area as swollen and tender, just as if you had suffered a sprain and its resultant swelling. Most patients may treat this discomfort with over-the-counter pain relievers, such as acetominaphin (Tylenol).
Remember, you should not treat any pain after your PRP therapy with NSAIDs (non-steroidal anti-inflammatory drugs) like naproxen and ibuprofen, as they will greatly interfere with the therapy.
A few patients may experience significant post-procedural pain, possibly due to the enhanced inflammatory action that PRP therapy promotes.
Most importantly, the patient must be … well, patient. PRP will not provide immediate relief from pain. The process of regenerating healthy tissue via PRP will take weeks to complete. Yet, this is an improvement over the months that may be required for the body to effect tendon or ligament repair without the added boost of platelet-rich plasma.
Article written by: Rob Williams, MD
Learn more by downloading our FREE eBook on PRP Therapy here:
To request an appointment or request more information for PRP therapy right here in Corpus Christi, just click the button below!
Dr. Williams has been practicing orthopedic surgery in Corpus Christi since 1998. After graduating from Texas Tech hereceived his medical degree from the University of Texas at San Antonio. At the prestigious Campbell Clinic located at the University of Tennessee, Dr. Williams completed not only an Orthopedic Surgery Residency, but an additional year of Fellowship Training in Spine Surgery. Dr. Williams is dedicated to creating an excellent patient experience in the office or in the surgery suite.
Topics:



