WHAT IS SPINAL STENOSIS? (SIGNS, SYMPTOMS, AND CAUSES)
June 10th, 2017 | 3 min. read


Spinal stenosis is a term used to describe a narrowing of the spinal canal—usually in the lower back or neck. Stenosis is a condition which can have different causes. If you have spinal stenosis, you may notice pain and other symptoms—but it’s possible you won’t have any clear symptoms, at least not at first. Onset can be gradual. A doctor’s visit and X-ray will be required to confirm the condition.
WHAT IS STENOSIS?
As a medical term, the word stenosis refers, generally, to the irregular narrowing of any passage within the body. Spinal stenosis is a narrowing of the spinal canal—the long, vertical cavity created by the stack of 33 vertebrae that make up the spinal column.
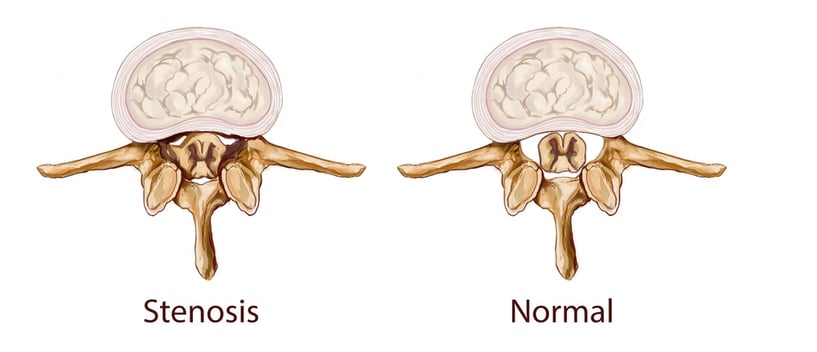
This space inside the vertebrae contains the spinal cord, which connects the nerves of the body to the brain. When the spinal canal becomes narrower due to damage or disease, the resultant crowding can sometimes lead to bone or tissue putting pressure on the spinal cord and the nerves that branch off from it. This pressure can result in symptoms like pain and numbness.
Stenosis can also affect the spaces through which nerve bundles and individual nerves pass as they exit the spinal cord.
HOW SPINAL STENOSIS OCCURS (CAUSES)
For the majority of people with spinal stenosis, the condition is age-related. If you are over 50, stenosis is most likely the result of a natural degeneration (breakdown) of the vertebrae due to ordinary wear and tear.
How does that wear and tear on the back lead to a narrowing of the spinal canal? The specific cause behind spinal stenosis may be one of the following:
- Bone spurs or overgrowths. Bone-on-bone friction from osteoarthritis can prompt the vertebrae to create spiny growths called bone spurs (commonly seen in the feet). When the bone spurs on the vertebrae protrude into the spinal canal, they can put pressure on the nerves and spinal cord.
- Herniated discs. Sometimes, a cushiony vertebral disc between two backbones suffers a stress injury called a herniation (often referred to as a rupture). A herniation means the jelly-like interior of the disc has protruded out a crack or split in the disc wall. This protrusion then bulges into the spinal canal. Disc herniations can happen to anyone due to sudden force or injury, but they become more common as we age, due to our cartilage becoming drier and more prone to fissures and tears.
- Ligamentum flavum hypertrophy (thickened ligament). A ligament called the ligamentum flavum runs down the back inside of the spine’s facet joints, connecting the vertebrae together. Sometimes this ligament may swell or grow thicker and reduce the overall space available in the spinal canal. This isn’t always a problem, but in combination with a slipped or herniated disc or bone spurs, this thickened ligament may contribute to an overall compression of the spinal cord and nerves.
- Ligament ossification (hardened ligament). A ligament called the posterior longitudinal ligament travels up and down the spine, inside the back of the spinal canal. If too many calcium deposits build up on this tissue, it can ossify, or turn to bone. The bony buildup can protrude into the spinal canal, reducing the available space.
- Paget’s disease. This bone disease can lead to oversized bone or excess bony growths throughout the body, including (and especially) along the spine. These growths and changes to the bone structure can crowd the spinal canal.
- Spinal trauma. Injuries to the spine (or to the surrounding bone or tissue) may cause swelling that can put pressure on the spinal cord. Dislocations and fractured pieces of bone may also enter the canal.
- Spinal tumors. A growth inside the spinal cord itself or in the area around it may reduce the space between the cord and the vertebrae. The bones of the spine itself may also be affected by bone loss or displacement by the tumor.
- This condition involves a vertebra sliding out of proper alignment; essentially, it slips forward onto another vertebra. This can happen as the result of an accident, an inherited condition, or a degenerative disease. The subsequent misalignment can put pressure on the spinal cord and nerve roots.
SIGNS & SYMPTOMS of spinal stenosis
Spinal stenosis may not show any symptoms at first. Onset can be gradual, worsening with time to include the following.
Cervical stenosis (neck)
- The most common symptom: numbness, weakness or tingling in the hand
- Numbness, weakness, or tingling in a leg, foot, or arm
- Balance problems when standing or walking
- Incontinence (bowel or bladder), due to nerves being affected by pressure on the spinal cord
Lumbar stenosis (lower back)
- Pain or cramping in the legs when walking or after standing for a sustained period of time. The pain improves when sitting or bending forward at the waist.
- Pain traveling down a leg
WHO GETS SPINAL STENOSIS?
Mostly, people over age 50.
If you’re under age 50, you may develop this condition, though it’s less likely. Some people are born with a narrower than average spinal canal, and this puts them at risk. In younger people, early onset arthritis can be a cause, as can scoliosis—the curvature of the spine may compress or stretch ligaments and put pressure on nerves and tissue. Certain genetic diseases affecting the spine may also be the cause (for example, the inherited condition achondroplasia, a form of dwarfism).
In athletes or those who work very physical jobs, an unusual amount of wear and tear on the back can also hasten the onset. Many professional athletes have been diagnosed with this potentially career-ending condition, including baseball players David Wright (New York Mets) and Lenny Dykstra (Philadelphia Phillies).
SUMMARY
If you suspect spinal stenosis, it’s important to visit a doctor and be examined. In rare cases, this condition, when left untreated, may progress and cause permanent, serious damage like incontinence, loss of sexual function, balance problems, weakness, and paralysis.
Contact Coastal Orthopedics in Corpus Christi, Texas for more information at (361) 994-1166.
Article written by: Rob Williams, MD
Dr. Williams has been practicing orthopedic surgery in Corpus Christi since 1998. After graduating from Texas Tech hereceived his medical degree from the University of Texas at San Antonio. At the prestigious Campbell Clinic located at the University of Tennessee, Dr. Williams completed not only an Orthopedic Surgery Residency, but an additional year of Fellowship Training in Spine Surgery. Dr. Williams is dedicated to creating an excellent patient experience in the office or in the surgery suite.
Topics:

