Herniated Disc Treatment Options: Surgical vs. Non-Surgical
May 18th, 2017 | 5 min. read
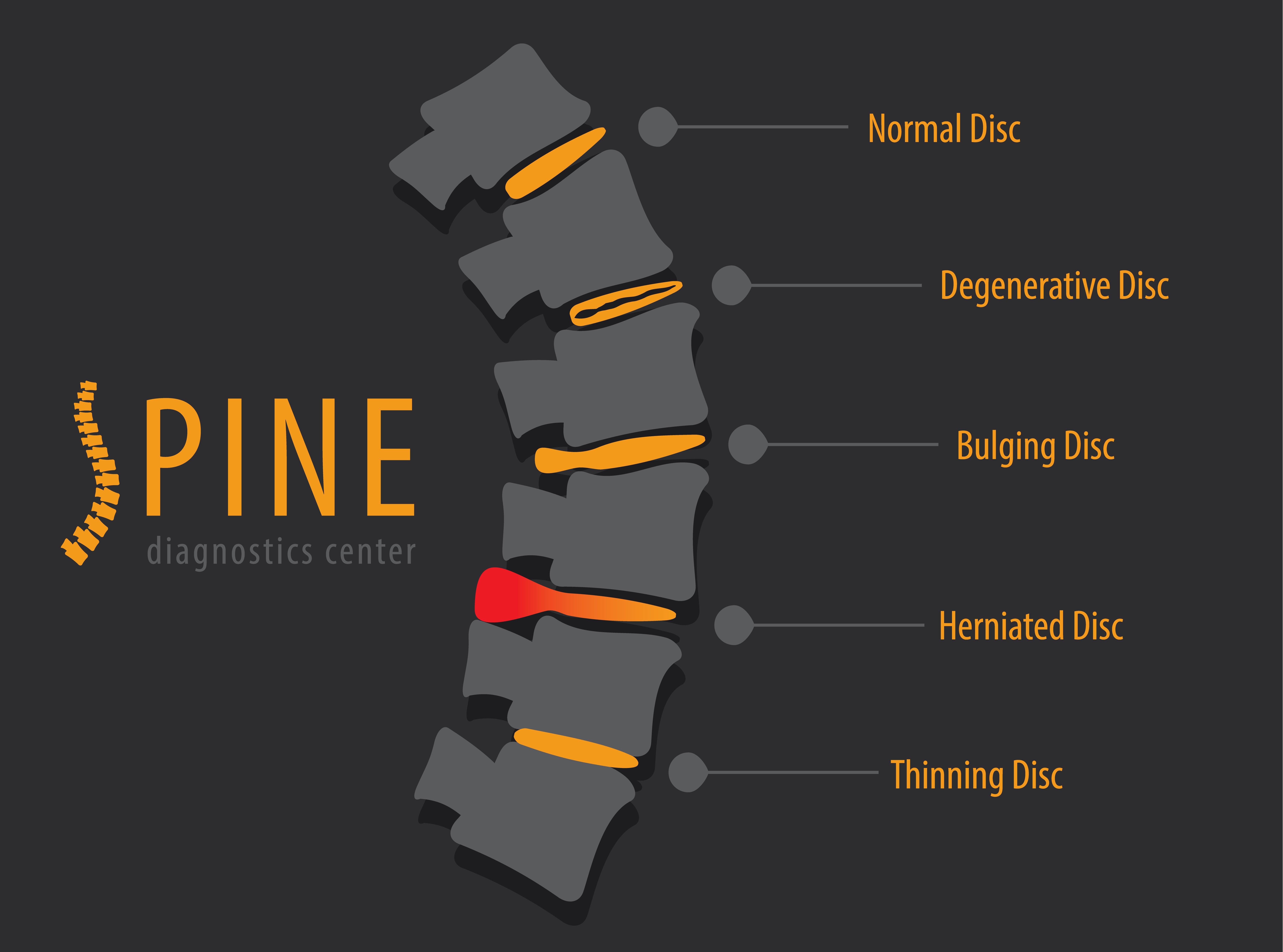
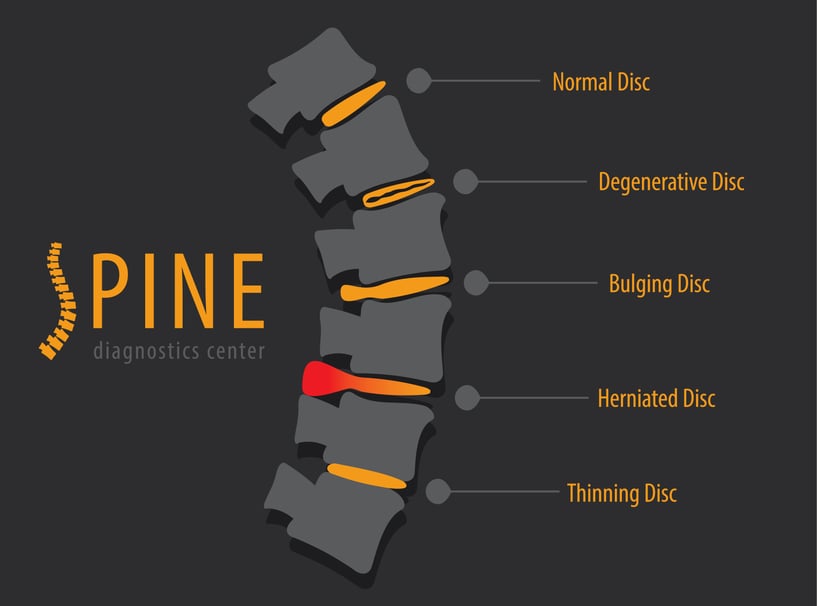
According to several studies, you may have some form of disc disorder—and not know it.
Some estimates claim as many as two-thirds of all people age 45 and over have some form of disc disease. Among the names for these conditions are herniated discs, slipped discs, bulging discs, torn discs, ruptured discs, black discs, collapsed disc, disc protrusion, etc., all of which are used more or less interchangeably.
Fortunately for all the middle-aged people in the world, most disc disease does not cause any noticeable pain, and does not require any medical treatment.
However, that still leaves millions of people with classic symptoms of herniated discs: pain, numbness, tingling, weakness, and more.
Modern medicine has developed several approaches to the treatment of a herniated disc, both non-surgical and surgical. Whichever path you choose to treat you aching neck or back will depend on your unique condition: what is causing the pain, where the pain is located, and what symptoms are manifesting.
Anatomy of a Herniated Disc
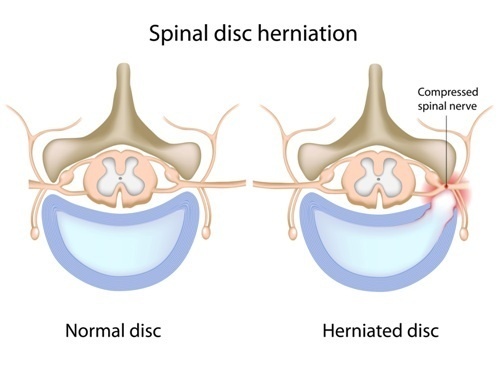
Discs are located within the spinal column, which is made up of 23 alternating discs and 33 bones (vertebrae). The vertebrae provide structural strength, stability, and protection for the spinal cord, the nerve fibers that run directly into the brain stem. The discs, which are made up of thick, rubbery cartilage, provide for flexibility, proper intervertebral spacing, dynamic alignment of the whole spine, and shock absorption.
The outer layer of each disc (the annulus fibrosis) surrounds a core of thick gel (the nucleus pulposus), which allows the discs to squash, stretch, and twist with the body.
A herniated disc occurs when the outer layer of the disc is torn, and allows the inner core to leak out. (In medicine, “herniation” is defined as “the abnormal protrusion of a body organ or other tissue through an opening in its surrounding membrane, muscle, or bone.”)
The leaking gel may irritate nerves within the outer layer of the disc itself, or, should it leak (herniated) completely out of the annulus fibrosis, it may compress, pinch, and irritate the spinal nerves running past.
Most slipped discs occur in the lower back. Bulging discs are also common in the neck. The most common symptoms that accompany a herniated disc are pain, numbness, tingling, and weakness that may spread to the arm or leg closest to the affected area. A slipped disc in the lower back may cause sciatica, pain running from the spine sometimes all the way to the toes.
Herniated Disc Treatment Options
An MRI is required to definitively locate and diagnose a herniated disc, as the soft tissues cannot be seen clearly on an X-ray. In addition, a doctor will need to ask specific questions about the severity, source, and symptoms of the pain being felt before beginning any course of treatment.
For most patients with slipped discs, doctors will recommend a conservative, non-surgical approach. This is due to several known facts about herniated discs:
- Not all herniated discs cause pain or symptoms.
- Back pain may be caused by injury, damage, or other issues with other soft tissues, such as muscles, tendons, and ligaments.
- Surgery may be equally or less effective than time, internal musculoskeletal adjustments, improved posture, or lifestyle changes, such as losing weight or strengthening back and abdominal muscles.
- Surgery may worsen the issue, or cause additional complications.
Unless a patient is suffering severe, disabling issues, such as major, advancing weakness in their limbs due to the damaged disc causing severe pinching of a nerve root (which may cause permanent nerve damage), sudden loss of control of their bowels or bladder, or crippling pain, the following non-surgical options will be the first step in treating the pain of a ruptured disc.
Treatments for a slipped disc will be the same regardless of the location of the herniated disc, should it occur in the neck (cervical), upper back (thoracic), or lower back (lumbar) area.
Nonsurgical Treatment Options for Disc Herniation
Non-surgical treatments of slipped discs will take four to six weeks for maximum effect. These approaches are designed reduce pain and discomfort, as well as to serve as ongoing diagnostic tests to pinpoint the precise nature of the disc damage.
Some “trial and error” will be necessary in order to ascertain the most effective combination of treatments.
In addition, the nonsurgical approach may educate patients on the proper body mechanics that will ensure any further damage is avoided in the future. Proper lifting techniques, stretching, and flexibility exercises can all protect the discs from unnecessary “wear and tear.”
- Rest. The simplest and often most effective means of reducing aches and pains. As most disc disease does not cause
 pain, this may rule out the disc as the source of back or neck pain.
pain, this may rule out the disc as the source of back or neck pain. - Physical therapy. Exercise and stretching may help relieve pressure on the nerve root.
- Heat and Cold. Ice packs and heat wraps may loosen tight muscles, reduce swelling and inflammation, and ease symptoms.
- Medication.
- The most effective over-the-counter (OTC) medicines for pain relief are called NSAIDs (non-steroidal anti-inflammatory drugs). Ibuprofen and naproxen are generally more effective than aspirin and acetaminophen.
- For more severe pain, prescription narcotic pain medications such as codeine, morphine, etc. may be required.
- Steroids may be prescribed and administered by a doctor for more serious issues of inflammation and pain relief.
- Epidural injections for severe cases of pain and inflammation may be used.
- Manipulation, particularly low-velocity chiropractic manipulation, may be helpful for patients not experiencing neurological problems.
- Traction. This approach may physically ease pressure along the spinal column.
Surgical Options for Disc Herniation Treatment
If four to six weeks of conservative, non-surgical treatment does not resolve the problems, surgery may be the best alternative to treat the pain caused by a slipped or ruptured disc.
The single most common surgery to treat a slipped disc is a discectomy: the removal or part or all of the damaged disc. Following is a list of surgical options of treatment for a herniated disc:
- Anterior (front) Cervical (neck) Discectomy and Fusion: treatment for a herniated neck disc. A small incision is made in the front of the neck, and the surgeon removes part or all of the damaged disc. The disc may either be replaced with an artificial disc, or more commonly, a small bone plug is used to space and “fuse” the two vertebrae above and below the affected disc.
- Cervical (neck) Corpectomy: The surgical removal of the damaged disc, as well as part or all of the surrounding vertebrae. Requires additional hardware to be installed, such as a metal plate, screws, or bone grafts, to ensure the spine remains stable afterwards.
- Lumbar (lower back) Fusion: This procedure will eliminate the abnormal motion caused by a damaged disc. It requires making an opening either through the back or stomach (or both), removing the damaged disc, and inserting either a bone graft or artificial hardware (or both) to stabilize the spine and allow the body to “fuse” the surrounding vertebrae.
- Microdiscectomy / Microdecompression: A minimally invasive procedure, most often used to relieve leg pain (sciatica) caused by a herniated disc. Reaching under the affected nerve root, the herniated part of the disc is removed, freeing space within the spinal canal and relieving the pressure caused by the slipped disc.
- Artificial Disc Replacement Surgery or TDR (total disc replacement): Exactly what it sounds like: the removal of the damaged disc, restoring the proper spacing between the affected vertebrae, and inserting the artificial disc.
It is important to note that there is no guarantee that surgery will relieve the pain, discomfort, and other symptoms of a herniated disc.
It is likely that a combination of surgical and non-surgical solutions to the issue will provide the greatest relief and most successful results for those suffering from a slipped disc, ruptured disc, herniated disc, bulging disc, or any other disc-related ailments.
Please contact Coastal Orthopedics today in Corpus Christi, Texas if you'd like to learn more about your treatment options for a hernaited disc (361) 994-1166.
Article written by: Rob Williams, MD
Dr. Williams has been practicing orthopedic surgery in Corpus Christi since 1998. After graduating from Texas Tech hereceived his medical degree from the University of Texas at San Antonio. At the prestigious Campbell Clinic located at the University of Tennessee, Dr. Williams completed not only an Orthopedic Surgery Residency, but an additional year of Fellowship Training in Spine Surgery. Dr. Williams is dedicated to creating an excellent patient experience in the office or in the surgery suite.
Topics:

