Rotator Cuff Tendinopathy: Treatment and Management
September 18th, 2017 | 4 min. read
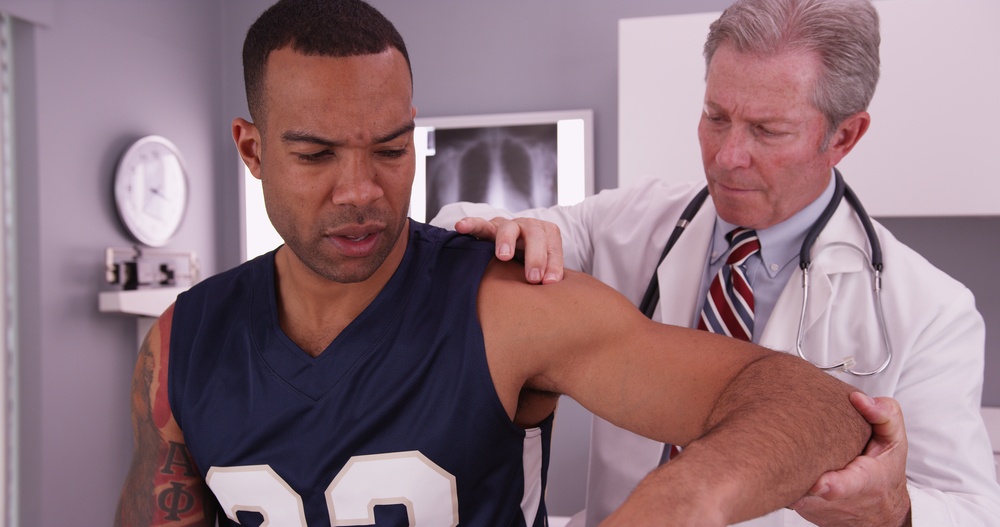
If you have rotator cuff tendinopathy (also called tendinopathy of the shoulder), you have cellular level degeneration of the tendon collagen in the rotator cuff of the shoulder. This degeneration can lead to chronic weakness, pain, limited range of motion and inflammation.
The breakdown of collagen from tendinopathy can’t be reversed, but the progression and symptoms of your chronic tendon disease can be managed through a combination of therapies and approaches.
First Step: Diagnosing Tendinopathy
Before you begin tackling a treatment or pain management plan for your shoulder tendinopathy, you need a physician to diagnose the condition.
The physician will begin by checking for one or more of these rotator cuff tendinopathy symptoms:
- Dull or gradually increasing, your pain may get worse when:
- lifting your shoulders above 90 degrees (for example, when throwing a baseball, swimming, or playing racket sports like racquetball or tennis)
- lifting objects
- reaching your arms behind your back
- sleeping on your side
- Gradually increasing over time.
- Stiffness/loss of range of motion. Gradually getting worse over time. This may be accompanied by a creaking feeling or a clicking sound when you rotate the shoulder or raise your arm.
- Tenderness or swelling. Though not all tendinopathy involves inflammation, sometimes this can be a symptom. When you press on your shoulder, the affected tendon may also feel thicker.
Your physician will also take into account any risk factors for shoulder tendinopathy, such as previous shoulder injuries, sports activities, occupational risk, age, obesity, or diabetes. (If you are over 40, are significantly overweight, or participate in an overhead throwing sport like baseball or tennis, you’re at greater risk.)
After looking at symptoms and risk factors, the next step is a physical exam—including diagnostic tests—to determine the cause of your symptoms.
Exams start with the doctor checking your range of motion, pain level, and the strength or weakness of your shoulder. To check for rotator cuff tendinopathy, your physician may ask you to move your arm through a series of movements. He or she may also feel your neck to check for signs of arthritis or a slipped or pinched disk—conditions that could be responsible for the symptoms you’re experiencing.
To confirm a diagnosis of shoulder tendinopathy, however—and to isolate its cause—your physician will probably need to do some imaging tests. For example:
- X-rays. X-ray imaging can determine whether a bone spur may be causing friction in your shoulder joint. A bone spur could be damaging or inflaming the tendons of the rotator cuff. Removing the spur may help to alleviate your symptoms.
- Ultrasound or MRI. These scans look at the soft tissue of the shoulder. They can help to determine whether you have any tears or inflammation in the rotator cuff tendons. If you do have tears or inflammation, these may be treated with some combination of rest, medication, exercise/physical therapy and surgery.
An exam can also diagnose or rule out other shoulder issues such as a shoulder dislocation, shoulder impingement, a SLAP lesion tear, a rotator cuff tear, tendonitis (which is similar to tendinopathy, but not chronic), frozen shoulder, or shoulder bursitis.
Learn more about rotator cuff surgery
Next Step: Non-Surgical Treatment of Rotator Cuff Tendinopathy
Most physicians will advise conservative, non-surgical treatment for tendinopathy, unless the degeneration of the tendon is severe and has resulted in a serious tendon tear requiring repair.
The purpose of non-surgical treatment is to find ways to reduce inflammation if you have it; to manage your pain; and to improve your range of motion, restoring it to normal if possible.
It bears repeating that chronic rotator cuff tendinopathy isn’t something that can be fixed or cured, per se; it’s caused by a cellular breakdown of the collagen in your tendons that’s usually due to sports-related or age-related wear and tear. However, treatments can manage your pain and other symptoms and may help to slow the degeneration (particularly if the degeneration is compounded by poor biomechanics when you’re using your shoulder joint).
The techniques available to manage tendinopathy non-surgically include:
- Stop or cut back on activities that contribute to the trauma in your damaged rotator cuff. If you’re an athlete (especially a baseball pitcher), you may need to go on the disabled list until your symptoms improve. Rest and avoiding activities that cause pain allows your body the opportunity to self heal.
- Use cold therapy in the form of ice packs applied to your shoulder several times a day. Cold helps to reduce inflammation and swelling.
- Taking over-the-counter anti-inflammatory medication like ibuprofen or naproxen can help to reduce swelling and fight pain. Prescription NSAIDs are also available. Talk to your doctor before beginning any long-term treatment with these pills, as they can have side effects and interactions with other drugs.
- Bracing/support. If your tendinopathy includes a minor tear or other acute injury, kinesio taping or wearing a sling may help to protect the injury while it heals.
- Exercises/massage. Passive and active exercises designed to strengthen and stretch the muscles around your shoulder can help to support the rotator cuff, taking some of the burden off damaged tendons and improving range of motion. Physical therapy may also improve postural issues or biomechanics mistakes that may be contributing to your shoulder pain or tendon damage.
- Other therapies. Electrical stimulation (e-stim), dry needling, and certain types of massage may help to break up adhesions between tissue, improving range of motion in the shoulder. These won’t reverse collagen degeneration, but they may help related tendon or muscle issues that may be affecting how you move and use the shoulder joint.
- Ongoing care of your shoulder. An orthopedist or physical therapist can help you with specific guidance. You may be urged to avoid lifting heavy items over your head. Don’t carry a heavy bag on one shoulder. If you’re using your shoulder joint a lot (for example, while playing sports or at work), take breaks throughout the day and stretch regularly. Sitting and standing with proper posture may help—at work, check your desk for the ergonomic setup. An ongoing shoulder care regimen may also be beneficial. A shoulder care exercise routine would include strengthening and stretching specifically designed to improve range of motion and make the shoulder stronger.
- Steroids injected into the affected tendon may help to ease rotator cuff pain and inflammation. However, these cannot be used more than a few times per year. Too many steroid injections can actually weaken tendons, making them more prone to acute injuries like tendinitis and ruptures.
Surgical Treatment of Rotator Cuff Tendinopathy
Surgery may be recommended if your symptoms do not improve with nonsurgical therapies after a period of time (usually 3-6 months).
If you’re referred to an orthopedic surgeon, arthroscopy—minimally invasive surgery involving the insertion of a camera through a small incision point—may be necessary to get a closer look inside the rotator cuff.
Once inside the joint, the surgeon may be able to see a problem that was difficult to identify on imaging tests. Impingement, for example, may require decompression surgery to remove impediments and make more space for the tendon to smoothly glide without friction.
Often, patients who progress to the point of needing surgery for tendinopathy actually have some other issue at play, such as a rotator cuff tear. Once the tear is repaired and the rehabilitation is complete, patients can usually return to prior activities.
To learn more about your treatment options for Rotator Cuff Tendinopathy, contact Coastal Orthopedics in Corpus Christi today at (361) 994-1166.
Article written by: Rob Williams, MD
Dr. Williams has been practicing orthopedic surgery in Corpus Christi since 1998. After graduating from Texas Tech hereceived his medical degree from the University of Texas at San Antonio. At the prestigious Campbell Clinic located at the University of Tennessee, Dr. Williams completed not only an Orthopedic Surgery Residency, but an additional year of Fellowship Training in Spine Surgery. Dr. Williams is dedicated to creating an excellent patient experience in the office or in the surgery suite.


