Most Common Sports Injuries for Women
May 30th, 2016 | 5 min. read

Statistically, men and women sustain sports injuries at about the same rate; but how they get injured, and why, are not exactly the same. Are you familiar with the most common sports injuries for women?
Though girls and boys are similar in childhood, puberty brings about hormonal and anatomical changes in women and men. These changes lead to physical differences in men's and women's bodies and how they perform in sports.
Alignment, form, physiology, body composition (muscle vs. fat), and performance diverge when we become adolescents. Men become prone to certain types of sports injuries like cardiovascular events, hernias, and back problems.
Women's injuries, on the other hand, more often relate to bone weakness or loss (osteoporosis) and the specific biomechanics of female bodies, particularly the shoulders, legs, knees, and feet.
sports injuries commonly affecting women
Post-puberty, adult women athletes are at risk for bone loss (osteoporosis), menstrual problems, and calorie depletion (with or without an eating disorder).
If you are a woman who exercises or trains more than 12 hours per week, you may develop all three issues simultaneously — what some researchers call the "female athlete triad." This triad can make you more prone to bone loss and subsequent physical injuries like bone breaks and stress fractures (see below).

Women are also more likely to experience knee and foot problems.
Many women, for example, have flat or pronating (rolling inward) feet, which can contribute to a condition called Miserable Malalignment Syndrome (MMS). MMS involves alignment and rotation of the quadriceps and knees relative to the hips. Misalignment can put undue pressure on tendons and ligaments, leading to knee pain or kneecap displacement.
How do these factors affect women who play sports? Below is a list of the most common musculoskeletal injuries affecting female athletes — why they occur and how to treat them.
Concussions (concussive brain injuries)
A concussion is a traumatic brain injury caused by a blow to the head or a jolt to the body that causes the brain to move rapidly or even twist within the skull. Concussions can lead to brain cell damage and chemical changes in the brain.
Recent studies indicate that women sustain concussions at a higher rate than men. The reasons are not yet clear, but researchers believe hormonal differences may be partly responsible for women's sensitivity to brain injury. Women also have less isometric neck strength and girth, which may make the head more vulnerable to sudden movements.
To prevent concussion:
- Avoid direct contact with other athletes when playing sports, if possible.
- Be alert to tripping hazards that may cause a fall.
- If your sport uses stunts (for example, in cheerleading), use spotters.
- If your sport requires diving (for example, in volleyball), learn safe techniques that avoid hits to the head.
- Wear a helmet if you can.
To treat concussion:
- Rest from all activity.
- Take pain relievers (ask your doctor for guidelines).
- Closely monitor for nausea and vomiting or behavioral changes, which may indicate a more serious injury.
ACL ruptures and tears
Located in the center of the knee, the ACL controls rotation and forward movement of the shin bone. ACL injuries are sustained on impact or when making sudden jump landings, stops, or pivots.
Because women land differently than men, in a more upright position, they are more likely to injure their ACLs (ACL injuries are three to six times more common in women).
To prevent ACL injuries:
As with any injury, no prevention method is 100% guaranteed; but some approaches can help to reduce your risk:
- Braces. Support braces may help to support ligaments and keep the knee from twisting over overextending.
- Technique. Women athletes can learn proper techniques to land in stable positions that protect the knee.

To treat ACL injuries:
- In the short term, RICE therapy and NSAIDs may help alleviate pain and swelling.
- Minor ACL tears may heal on their own with rest.
- For severe tears and ruptures, arthroscopic surgery may be recommended by an orthopedist.
- In cases where significant damage to the joint has been sustained, a doctor may recommend a total knee replacement.
Patellofemoral syndrome ("runner's knee")
Runner's knee (or "jumper's knee") is a common condition in females and young adults who participate in sports, though even nonathletes can develop this condition.
Patellofemoral syndrome is characterized by soreness in the front of the knee and around the patella (kneecap). Symptoms include pain and stiffness that may make it difficult to climb stairs or kneel.
Many women have MMS and kneecap alignment issues, making them more prone to developing runner's knee. In athletes, runner's knee can also result from overuse and overtraining.
To prevent patellofemoral syndrome:
- Change your activity level gradually.
- Use proper sports training techniques.
- Check your footwear and equipment to ensure proper fit.
To treat patellofemoral syndrome:
- Reduce your activity level if possible, or cross-train to reduce stress on the knee.
- NSAIDs, RICE, and compression can be used for pain and swelling.
- Physical therapy can stretch and strengthen the knee and surrounding muscles.
- Braces and foot orthotics may be prescribed by an orthopedist for ongoing support.
Plantar fasciitis
A band of connective tissue called the plantar fascia runs along the sole of the foot, connecting the heel bone to the toes. Sometimes when the fascia gets overstretched it develops tears that cause pain, inflammation, and stiffness, usually under the heel.
Women are more prone to plantar fasciitis than men. Athletes may get plantar fasciitis if they have flat feet or unusually high arches, if they are on their feet for many hours, or if their calf muscles are too tight.
To treat plantar fasciitis:
- Stretch the calves, Achilles tendon, and the bottom of the foot.
- Massage therapy may bring some relief.
- Foot orthotics (supports inserted into the shoes) prescribed by an orthopedist may help.
- Surgery is a possibility when the condition does not respond to other techniques.
Shin Splints (Medial Tibial Stress Syndrome, or MTSS)
Shin splints is a term to describe anterior (frontal) lower leg pain caused by overtraining. Women are more likely to develop shin splints than men, and are about three times as likely to see their splints develop into stress fractures.
To treat shin splints:
- Rest. If you must exercise, try a lower impact alternative while you recover, such as swimming.
- Ice your leg.
- Stretch your Achilles and calves regularly.
- Make sure you're wearing proper footwear.
Rotator cuff (shoulder) injuries
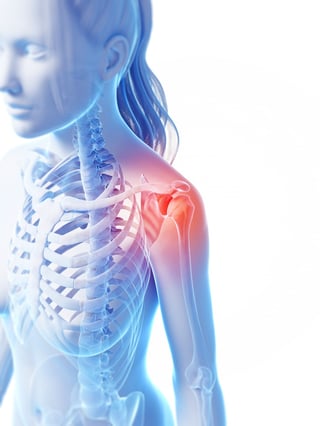
Rotator cuff tears and degeneration are often the result of age and overuse. However, in women athletes, these injuries can be the result of repetitive actions (such as reaching upward or completing a swimming stroke) or falling on an outstretched hand (for example, when diving in volleyball).
Women are more prone to shoulder injuries than men. This may be caused by greater shoulder instability due to less upper body strength, weaker rotator cuffs and periscapular muscles, and looser supporting tissues.
To prevent shoulder injuries:
- Use weight training to strengthen the muscles of the shoulder, upper back, and arm. (See a sports medicine expert or orthopedist for recommended exercises.)
- Stretch regularly to maintain flexibility.
To treat shoulder injuries:
- Rest and, if directed by an orthopedist, immobilize the shoulder.
- Use NSAIDs or topical pain reducers.
- Strengthen the joint with physical therapy exercises prescribed by an orthopedist or expert in sports medicine.
- Shoulder surgery (such as arthroscopy) may be necessary in some cases.
Stress fractures
Stress fractures are overuse injuries to the bone caused by muscle fatigue. Due to a loss of bone mass that begins around age 30, women are more likely than men to get stress fractures, particularly in the lower legs and feet. Training too rigorously too quickly (as opposed to gradually increasing over time) also increase your risk of injury.
Other contributing factors include being too lean or eating too restrictive a diet. Some women, particularly endurance athletes like long distance runners, can develop menstrual abnormalities that reduce estrogen levels in the body. Too little estrogen can weaken the bones, making them more prone to injury.
To prevent stress fractures:
- Eat enough calories, especially if you are active.
- Consume foods high in bone-building nutrients like calcium, vitamin D, vitamin K, vitamin C, magnesium, and iron.
- Gradually increase your training intensity over time.
To treat stress fractures:
- Refrain from weight-bearing activities until your fracture heals (usually, six to eight weeks).
- Take NSAIDs and use RICE treatment as needed.
- If your fractures come back, your orthopedist may recommend shoe inserts or braces.
- For severe fractures or fractures that won't heal, visit an orthopedist to talk about fracture care management or bone growth stimulation.
Sports that cause the most injuries for women

Generally, the sports and activities that seem to report the most injuries to women include:
- Basketball (ACL, concussions)
- Cheerleading/Dance (ACL, stress fractures)
- Gymnastics (herniated discs, tendinitis, wrist and ankle sprains)
- Lacrosse (ACL, concussions)
- Running/Track and Field/Cross Country (ACL, stress fractures)
- Soccer (ACL, concussions)
- Softball (rotator cuff, shoulder)
- Swimming (rotator cuff, shoulder)
- Volleyball (ACL, rotator cuff, shoulder)
The bottom line: sports injuries happen; no physician can guarantee you will not get injured at some point. However, with proper training techniques, equipment, and awareness, you can minimize your risk of some of the most common sports injuries affecting women.
If you are injured, an orthopedic specialist can help to assess your condition and prescribe a rehabilitation plan to get you back into the game. Give Coastal Orthopedics located in Corpus Christi, TX a call and ask for a consultation. Telephone: 361.994.1166.
Article written by: Rob Williams, MD
Dr. Williams has been practicing orthopedic surgery in Corpus Christi since 1998. After graduating from Texas Tech hereceived his medical degree from the University of Texas at San Antonio. At the prestigious Campbell Clinic located at the University of Tennessee, Dr. Williams completed not only an Orthopedic Surgery Residency, but an additional year of Fellowship Training in Spine Surgery. Dr. Williams is dedicated to creating an excellent patient experience in the office or in the surgery suite.
Topics:

